Asthma is most common respiratory tract infection. It is the reversible obstruction of large and small airways.
Pathophysiology
Bronchial asthma is characterized by hyperresponsiveness of tracheo-bronchial smooth muscle to a variety of stimuli, resulting in narrowing of air tubes, often accompanied by increased secretions, mucosal edema and mucus plugging.
- Inflammation
- Hyper reactivity
- Bronchospasm
Bronchial hyper reactivity results in inflammation of bronchial wall because of increased leakiness from micro circulation, leading to edema of bronchial wall.
Because of leakage, there is plugging of bronchi with thick mucous, symptoms include wheezing breathlessness.
Parasympathetic innervation is present in fibers of walls of bronchi, when inflammation occurs, increased parasympathetic tone due to release of acetylcholine leads to bronchospasm.
Vascular smooth muscle has sympathetic innervation. Increased pulmonary blood flow occurs because of vasodilatation, ultimately leading to bronchodilatation.
Hyper reactivity is due to release of chemical mediators.
Mediators are also released from certain cells, storage granules, besides certain other cells are recruited including eosinophils, neutrophils, monocytes, which themselves release mediators contributing to inflammatory response.
The strategy these days is to address inflammation.
Phases
2 phases are present:
- Immediate –release of histamine leading to antigen-antibody reaction on surface of mast cells
- Late
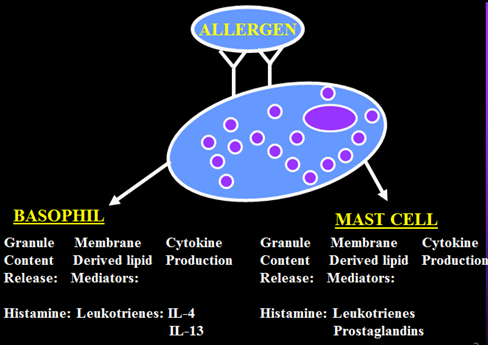
IgE antibodies are synthesized within mast cells in lungs. Antigen interacts with IgE on mast cells leading to release of mediators.
IL 4 and IL 13 are mainly responsible for bronchoconstriction and bronchospasm.
Mast cells release platelet activating factors, responsible for late phase eosinophilia.
For control of asthma, antihistamines are least beneficial especially exercise induced and allergic asthma and should be avoided. Normally leukotriene antagonists are given because:
- Leukotrines are contributing more in process
- Antihistamines cause more dryness
Bronchial inflammation differs because here hyper reactivity is the main problem.
Main goal is to treat underlying inflammation by use of anti inflammatory drugs.
Types of Bronchial Asthma
1. Extrinsic Asthma: (allergic)
It is mostly episodic, less prone to status asthmaticus
- Atopic (immediate due to IgE antibody).
- Nonatopic delayed for some hours, associated with production of precipitating antibodies
2. Intrinsic Asthma
It tends to be perennial, status asthmaticus is more common. Associated with COPD.
Classification
2 groups are present:
- Bronchodilators/relievers –address acute phase
- Anti inflammatory/controllers –address undelying
Bronchodilators
Sympathomimetics:
- Salbutamol, Albuterol
- Terbutaline,
- Bambuterol,
- Salmeterol,
- Formoterol.
b. Methylxanthines:
- Theophylline (anhydrous) (oral preparation with erratic solubility)
- Aminophylline
500 mg diluted in 5% dextrose is given I/V very slowly, as can cause tachycardia, arrhythmias, having less therapeutic index.
c. Anticholinergics:
- Ipratropium bromide (given inhalational, adjuvant therapy)
- Tiotropium bromide
Leukotriene Receptor Antagonists
- Montelukast,
- Zafirlukast
These are 1000 times more potent mediators, they treat underlying infection, breakthrough for children.
Mast Cell Stablizers
- Sodium cromoglycate,
- Nedocromil,
- Ketotifen (5HT action)
Corticosteroids (main stay)
Systemic:
- Hydrocortisone,
- Prednisolone & others.
- Beclomethasone dipropionate,
- Budesonide,
- Fluticasone- propionate,
- Flunisolide
Anti –IGE Humanized Monoclonal Antibodies
- Omalizumab
Approaches to Treatment
- Prevention of antigen-antibody reaction- avoidance of antigen, hyposensitization – possible in extrinsic asthma and if antigen can be identified
- Suppression of inflammation and bronchial hyper reactivity (corticosteroids)
- Prevention of release of mediators (Mast cell stabilizers)
- Antagonism of released mediators (Leukotriene antagonists, 1000 times potent than histamines)
- Blockade of constrictor neurotransmitter, Acetylcholine (anticholinergics)
- Mimicking dilator neurotransmitter (sympathomimetics)
- Directly acting bronchodilators (Methyl xanthines)
Sympathomimetics
Short Acting
Salbutamol, Terbutaline
Long Acting
Formeterol, Salmetrol, Bambuterol
Preferentially directly into airways by inhalation.
Onset of action via inhalational route is 1-5 minutes. Action is for 2-6 hours.
Oral administration is not preferred for bronchodilation although having prolonged action, up to 8 hours. Also
- Systemic side effects are produced
- Metabolic side effects
Although some absorption occurs through inhalational route as well, but there is not much toxicity. Beta2 drugs given in syrup form in children under 5 or elderly chronic asthmatics with symptoms aggravating. Can be given orally. Albuterol syrup
Mechanism of Action
1. Beta-2 adrenoceptor agonist, when administered binds beta 2 receptors
- Stimulation of adenylate cyclase
- Increase cAMP
- Bronchodilation and decreased muscular tone
2. Increase potassium conductance leading to hyperpolarization and relaxation of bronchial muscle cells.
Terbutaline subcutaneous preparation is available. Usually beta 2 agonists are preferred in dyspnea with bronchoconstriction, providing symptomatic relief.
Short term drugs have quick onset of action. Salmetrol reduces possible bronchodilation for 12 hours.
3. Inhibit release of chemical mediators from mast cells, lymphocytes which have beta 2 receptors in different cells in lungs àincrease cellular cyclic AMP contributing to inflammation by preventing release of cytokines.
4. Mucociliary action -Increase mucus clearance by an action on cilia
Uses
- Acute asthma Inhalation/I/V (short acting drugs)
- Chronic Asthma/ Prophylaxis oral/Inhalation (long acting drugs)
Chronic treatment decreases receptor sensitization and decreases action of drug. Effective in young asthmatics, but desensitization is not observed in beta 2 receptors present on bronchial smooth muslces (resistant). Desensitization is cell specific.
Beta 2 receptors on mast cells are desensitized.
- COPD (less benefit due to toxicity)
- Salmetrol also has anti inflammatory action. It acts on eosinophils. As controller Salmetrol can be added to corticosteroids, dose of which is decreased when combined.
There is risk of side effects due to genetic variations in beta 2 receptors. Patients homozygous for arginine genotype especially African-Americans. Salbutamol, Salmetrol have greater risks, affecting transcription, increasing the mortality rate.
Methylxanthine
Aminophylline, Theophylline
Theophylline is least expensive, very old drug and effective.
It is ethylated xanthine (dioxy purine) structurally related to uric acid.
Solubility of methyl xanthine is low and is enhanced by formation of complex with ethylene diamine in 1:1
Theophylline + Ethylene diamine = Aminophylline
Mechanism of Action
1. Inhibit Phosphodiestrase Enzyme (which catalyzes breakdown of cAMP). Many isoenzymes are present but isoenzyme III and IV are most effective.
- Increase cAMP
- Dephosphorylation of MLC
- Bronchodilation
2. Translocation of intracellular calcium
- Increased intracellular calcium lead to increased diaphragmatic contractility
3. Blockade of adenosine receptors
- Decrease contractility of bronchiolar smooth muscles
Uses
Drug is slowly given over 20-40 minutes, otherwise death occurs due to cardiac arrhythmias.
- Acute asthma- I/V (slowly)
- Chronic asthma (prophylaxis) Oral
- Treatment of apnea of preterm infants as metabolized in liver and:
- Converted in caffeine behaving as stimulant, which is exploited in treatment
- Volume of distribution is very large
- 2nd line drug in bronchodilation, having narrow therapeutic window.
Adverse effects
- Dose has to be maintained between 5-20 mcg/l, if it crosses 20 mcg/l severe CNS toxicity and convulsions occur.
- After 15 mcg/l GIT symptoms including pericardial pain occurs
- Tachycardia, palpitations
Drug monitoring is mandatory, given only in facilities having monitoring facilities.
Still theophylline is preferred in children over corticosteroids as growth retardation occurs by corticosteroids.
Sustained release preparations including 8 hourly, 12 hourly and 24 hourly preparations maintaining plasma levels for peak symptoms.
Pharmacokinetics
- Absorbed readily after oral administration, per rectal suppository has erratic absorption.
- Peak plasma concentration is achieved within 2 hours
- Volume of distribution is 0.4-0.6 l/kg, important fact is that infants have much larger Vd than adults.
Drug Interactions
Smoking, oral contraceptives, phenytoin, barbiturates increase clearance, dose adjustment is required.
In viral infections there are chances of toxicity as clearance is decreased.
Antibiotics, macrolides and cimetidine are not given with methyl xanthine as clearance is decreased
With Anti T.B drug rifampicin clearance of methyl xanthine is increased.
Anticholinergics
- Ipratropium
- Oxytropium
- Tiotropium
Selective in action, atropine is very potent but not selective so not used because of toxicity.
Mechanism of Action
- Blockade of muscarinic receptors present in bronchi and bronchioles
- Decrease mucus viscosity
- Increase mucociliary clearance
In therapeutic doses, does not overcome bronchoconstriction as non muscarinic in nature.
Given as aerosol inhalation.
In lungs relieves bronchospasm.
Duration of action is up to 5 hours.
Minimal systemic effects as poorly absorbed from lungs.
Uses
- Chronic asthma/prophylaxis (Inhalation) (More effective & less toxicity)
Limited role in asthma, main role is to decrease bronchoconstriction in bronchitis caused by stimulation of muscarinic receptors. Antibiotics are given for secondary infections.
Mainly for COPD.
Adverse effects
Dry mouth –since not as effective given in combination with beta 2 agonists and corticosteroids, when not controlled by beta agonists alone.
Leukotriene Receptor Antagonists
- Montelukast – oral
- Zafirlukast – (Cingular) oral administration for control of asthma
Leukotrines are products of arachidonic acid metabolism. They are released at the site of inflammation producing bronchoconstriction having contributory effect to inflammation and bronchoconstriction.
Mechanism of Action
Montelukast and Zafirlukast are competitive antagonists.
- Inhibits cysteinlyl leukotriene Cys LT1 receptor relieving bronchospasm and bronchoconstriction.
- Inhibit physiologic actions of LTC4, LTD4, LTE4
- One drug blocks synthesis of 5 lipooxygenase and is hepatotoxic Zileuton. Half like is 2.5 hours
When Montelukast is administered, it binds cysteine leukotriene 1 receptor
Uses
- Prophylaxis & chronic treatment (oral)
(Exercise, antigen, aspirin induced asthma)
Pharmacokinetics
- Half life 10 hours
- Bioavailability greater than 90%
- Peak plasma binding about 99%
- Both metabolized by cyt p450
- Montelukast is 60-70% metabolized, having plasma life about 3-6 hours.
Side effects
Rare.
- Inflammation at site in lungs
- Rarely hypersensitivity reaction
- Patients already treated with glucocorticoids have decreased dose.
- Chraug Stauss Syndrome
This is not due to drug but due to pre existing underlying disease, eosinophilia and vasculitis is seen.
Drug Interactions
Zafirleukast has drug interaction with warfarin sodium, leading to increased prothrombin time, thus dose has to be monitored.
Increase in theophylline levels, which is itself bronchodilator
Monteleukast is commonly used.
Mast Cell Stabilizers
- Na chromoglycate inhalation
- Nedocromil
- Ketotifen- (5HT action) oral
Nedocromil and Ketotifen are not bronchodilators, not having direct effect. They are ineffective once antigen antibody reaction takes place.
Mechanism of Action
- Inhibit transmembrance influx of Ca provoked by antigen antibody interaction on the surface of mast cells. this is prophylactic use and have to be given before antigen enters.
- Stabilize mast cells membrane and inhibit release of chemical mediators
- Depress exaggerated neuronal reflexes triggered by stimulation of irritant receptors
- Depress axonal reflexes which release inflammatory neuropeptides.
- Inhibit release of cytokines from T-CELLS
Only 5% sodium chromoglycate reaches lungs, rest get accumulated leading to irritation.
Allergic conjunctivitis –nasal sprays, eye drops
Uses
Prophylaxis of allergic exercise, irritant induced asthma.
Adjuvant therapy, dose limited.
Now limited role due to leukotrines, was drug of choice in children.
Corticosteroids
- Hydrocortisone I/V
- Prednisolone oral
- Betamethosone
- Beclomethasone inhalation
- Budesonide
- Flucitasone having affinity for glucocorticoids receptors in airways
Mechanism of Action
- Anti inflammatory action
- Decrease mucosal oedema, mucus secretion and reduce capillary permeability
- Stabilize mast cells
- Block immune response, decrease antibody formation
- Antagonise histaminergic and cholinergic responses
- Enhance beta-2 adrenoceptor responsiveness to agonists (Catecholamines)
Effects appear after 1 week, and it takes nearly 10 weeks for control of disease.
Beneficial effects are observed with inhalted 500 mcg.
Maximum therapeutic range is 500 mcg/ml.
Toxicity
Systemic toxicity occurs when steroid is inhaled, more than 1500 mcg.
Even with 500 mcg dose there are chances are
- Osteoporosis
- Dysphonia
- Oropharyngeal candidiasis
Uses and Routes of Administration
Bronchodilator is given immediately because:
- It takes about 1 week for effects to appear.
- Due to constriction, drug cannot reach lungs so bronchodilator is given
a. Acute severe asthma (status asthmaticus)
Hydrocortisone I/V
b. Acute asthma – oral
Prednisolone
c. Chronic asthma –(Prophylaxis) Inhalation
Beclomethasone etc
Ciclesonide
Prodrug, when absorbed drug is acted upon by esterases in bronchial epithelial cells, less amount of drug absorbed gets bound to glucocorticoid receptors, bones, skin, eyes, and there are less chances of osteoporosis and cutaneous thinning.
It has some role in people predisposed to cataract and osteoporosis.
Status Asthmaticus
- Status asthmaticus is an acute exacerbation of asthma that remains unresponsive to initial treatment with bronchodilators.
- It is a life threatening form of asthma, because it can lead to respiratory failure and cardiac arrest.
- Status Asthmaticus requires immediate treatment (corticosteroids are essential as immediate treatment)
- Air trapping strains on breathing muscle which are fatigue and exhausted
- Status asthmaticus is frequently associated with metabolic acidosis, and acidosis reduces the effectiveness of beta agonist.
- I/V NaHCo3 added if pH is below 7.5 in patient with refractory status asthmaticus, but there is risk of hypercapnia, in children.
- decrease in PCO2 level corrected with nasal/Face mask oxygen (Helium)
- Continuous nebulization of albuterol for the first few hrs
- Switched to intermittent albuterol very 02 hrs. I/V
- corticosteroids, inhaled ipratropium every 06 hrs
Treatment of last resort used in status asthmaticus include:-
- Providing G.A with inhaled anaesthetic which are potent bronchodilators.
- I/V ketamine, is also helpful.
- However help of an anesthesiologist is required.
CAN STATUS ASTHMATICUS BE PREVENTED?
The best way to decrease the possibility of having a severe attack is to take medication regularly as prescribed:-
- Never to stop taking inhaled steroids
- Leukotriene modifiers / “Controller” unless instructed to do so
Monoclonal Antibodies
Can be given to patients having severe forms of disease.
They bind to IgE antibodies present on mast cells. If administered I/V or subcutaneously, humanized monoclonal antibodies decrease levels of IgE antibodies, decreasing tendency of severe asthma, in both phases (immediate/delayed).
Also improve nasal/conjunctival symptoms, allergic manifestations. These are reserved for severe cases, if want to reduce dose of corticosteroids as there are undetectable levels of IgE antibodies in plasma and no antigen antibody reaction occurs.
 howMed Know Yourself
howMed Know Yourself





thank u for d lecture and reserch been an asthmatic i feel no more longly cos i have those that care remani bless