Fraction of the dose of a drug contained in any dosage form that reaches the systemic circulation in unchanged or active form administered through any route is known as bioavailability.
Drugs injected using intravenous route of administration have 100% bioavailability, while others have much less bioavailability, because:
- All of the drug may not be adsorbed
- Metabolism of the drug might occur before reaching the site of action
Drugs not absorbed by the oral route are highly polar drugs, thus have low bioavailability.
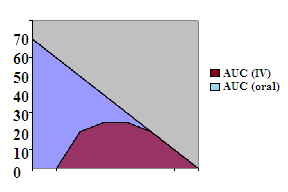
Bioavailability = AUC (oral)/ AUC (I/V) x 100
Where AUC is the area under the curve
X-axis represents time, while y-axis represents the plasma concentration.
Bioavailability is the ratio of the area calculated for oral route of administration to the intravenous route of administration. It is determined by comparing the plasma levels of a drug after administration with plasma drug level achieved by I/V injection.
Factors Affecting Bioavailability:
1. Route of administration
Drugs given by intravenous route have 100% bioavailability. Exception includes prostaglandins, which are inactivated/metabolized in the lungs, therefore, their bioavailability may be zero after I/V injection. Those given by intramuscular route have bioavailability less than I/V route but more than subcutaneous route, while subcutaneous route has bioavailability more than the oral route. Only 10% of the dose of digoxin reaches systemic circulation after oral administration because of lack of absorption and bacterial metabolism within intestines. Even some of the drugs given by oral route may have 100% bioavailability but this is rare.
By rectal route, half of the drug undergoes first pass metabolism.
Chloramphenicol, an antibiotic, administered by intravenous route has bioavailability less than oral route because it is present in pro form and has to be activated in the intestines.
| Route | Bioavailability | Characteristics |
| Intravenous | 100% | Most rapid |
| Intramuscular | 75≤100% | Large volume may be injected but painful method |
| Subcutaneous | 75≤100% | Smaller volume than IM, may be painful |
| Oral | 5≤100% | Convenient, first pass metabolism occurs |
| Rectal | 30<100% | Less first pass metabolism than oral route |
| Inhalation | 5<100% | Rapid onset |
| Transdermal | 80≤100% | Usually slow absorption, lack of first pass metabolism and prolonged duration of action |
2. Factors affecting absorption
Factors affecting absorption may be classified as those related to the drug and those related to the body. They have been discussed separately. If absorbance is decreased, bioavailability is decreased and vice versa. For a drug to be readily absorbed, it must be hydrophobic yet have some solubility in aqueous solution.
3. First pass metabolism
Pre systemic metabolism en-route from the route of administration to the site of action is known as the first pass metabolism. Most common site of first pass metabolism is the liver because after absorption the drug administered by oral route enters the portal circulation to reach the liver. First pass metabolism may also occur in the intestines, lungs adrenals or any other organ.
Significance:
- Drug undergoing first pass metabolism has low bioavailability, the dose must be adjusted keeping this in mind.
- If a person is undergoing a liver disease, bioavailability may be increased, because most drugs then enter systemic circulation in unchanged form. The dose must be decreased otherwise toxic effects might result.
Drugs undergoing first pass metabolism and sites:
a. Bronchial mucosa:
Prostaglandins, nicotine and isoprenaline
b. Intestinal mucosa:
Chlorpromazine, levo dopa, tyramine, alpha methyl dopa, testosterone and progesterone
c. Liver:
Glyceryltrinitrate, amitriptyaline, nortriptyaline, imipiramine, pentazocine, lignocaine, propanolol, labetalol, cimetidine and pethidine.
Glyceryltrinitrate is administered sublingually, by oral route it has almost 0% bioavailability.
Lignocaine is a local anesthetic and antiarythmic drug, its bioavailability by oral route is also 0%.
Highly polar drugs also have 0% bioavailability. They are not absorbed from the intestine. Examples include streptomycin and gentamicin.
Extraction Ratio:
The effect of first pass metabolism on bioavailability is measured by extraction ratio.
Extraction ratio = Clearance by liver/Hepatic blood flow
Where clearance is the amount of drug cleared from the unit plasma in unit time by liver.
Systemic bioavailability = Absorption x (1- Extraction ratio)
4. Chemical Instability
Drug may be destroyed by the HCl or enzymes present in the GIT. Benzyl penicillin is not given orally because it is destroyed by HCl. Parenteral route is generally preferred.
5. Quality control
Quality control is related mainly to different brands. One drug might be manufactured by different companies. These brands have different bioavailability although the drug is same. The difference lies in the manufacturing process.
a. Particle size:
Greater the size, smaller is the absorption. Size is inversely proportional to bioavailability. Small particle size is important for absorption of corticosteroids, chloramphenicol and griseofulvin.
b. Diluents/Excipients
Inactive ingredients which do not have pharmacological action. These are important when the drug is given in solid forms (tablets, capsules, pills). Drug before absorption must disintegrate and dissolute. Disintegration and dissolution may differ with different brands. If dissolution time is more, bioavailability will be less and vice versa.
These are added to:
- Increase bulk when dose is very low e.g. digoxin
- Adding stability, making drug resistant to environmental conditions
- Mask objectionable taste of drug
Excipients
Excipients are the inert substances added to the tablets or pills to increase their bulk because sometimes the dosage is very small.
Diluents
Diluents are inert substances used in case of liquids. Commonly used diluents include lactate, lactose, starch, sucrose, calcium phosphate.
Diluents and excipients may affect bioavailability of different brands. They may bind with the active principle. Sometimes when the patient is taking one brand for a very long time, suddenly bioavailability may change by changing the company.
c. Compression pressure
If tablets or pills are more tightly bound, the bioavailability is decreased.
d. Moisture content/Binding agents
Moisture content may act in two ways:
a. If the moisture content is more, disintegration time is less
b. Sometimes some drugs when have more moisture, form lumps in the stomach, which decreases their absorbance.
Thus moisture content may act both ways.
e. Polymorphism
When the drug is chemically same but different in arrangement of molecules, the phenomenon is known as polymorphism. Arrangement of molecules may be different with different brands.
Disintegration time:
The time in which a solid dosage form administered orally releases the active drug for absorption is called disintegration time.
Clinical Significance:
Bioavailability differs with the dosage forms. Drug in liquid form have more bioavailability than those of solids, while gases have the highest bioavailability. This is why inhalation is used in bronchial asthma.
With the same brand, dosage form manufactured by different companies may differ in bioavailability.
Three terms are generally used:
a. Bioequivalent:
If two similar drugs have the same bioavailability, they are called bioequivalent. If the two similar drugs do not have the same bioavailability, they are called non-bioequivalent.
b. Therapeutic equivalent
If two similar drugs perform the same effect, have same efficacy and toxicity, then they are called therapeutically equivalent.
c. Chemical Equivalent
If two drugs are manufactured according to the same principles and criterion layed down in pharmacopoeia (official book published by country to manufacture drugs in that country), then they are called chemically equivalent.
Two brands may be chemically equivalent but may not be bioequivalent and therapeutically equivalent because they might differ in the factors mentioned above.
Sensitive Drugs:
- Antimicrobials
- Anticonvulsants
- Corticosteroids
- Cardio active drugs
- Oral antidiabetics
- Chemotherapeutic agents for cancer
If patient is stabilized on one brand, it should not be changed, because if the bioavailability is decreased the drug will have less effect or if the bioavailability is increased, it might lead to toxicity.
Antimicrobials:
Anti tuberculosis drugs have to be continued for six to nine months. Recurrence of disease might occur on changing to brand with less bioavailability, although symptoms disappear after four weeks. Bacteria may also become resistant.
Anticonvulsants:
Anticonvulsant dose is adjusted by starting from a lower dose to reach the state where patient is free from fits. Drugs have to be continued for the whole life. If the brand is changed reappearance of convulsions might occur due to decreased bioavailability. Phenytoin is a drug of low therapeutic index. There exists small difference between toxic and therapeutic effects which must be taken care of.
Cardio active drugs:
Cardio active drugs like digoxin have low therapeutic index. Small changes in plasma levels may lead to toxicity.
Oral antidiabetic drugs:
Oral anti diabetic drugs have to be continued for the whole life. If bioavailability is increased, it may lead to hypoglycemia and fainting. Decreased bioavailability may cause hyperglycemia and diabetic complications.
Chemotherapeutics have low therapeutic index too. Plasma levels of corticosteroids matter as well.
We have to adjust the dose so that therapeutic failure does not occur.
Therapeutic Index:
Therapeutic index represents the safety of a drug. Drugs having large therapeutic index and safer and vice versa.
Therapeutic index = LD50/ED50 = TD50/ED50*
Where, LD50 is a dose which can kill 50% of the animals administered
ED50 is a dose which can save 50% of the animals
TD50 is the median toxic dose
ED50* is the median effective dose
Drugs having low therapeutic index include:
Anticonvulsants, lithium, anticoagulents, corticosteroids and cardio active drugs.
Therapeutic Window:
Therapeutic window is the range between the high therapeutic index and low therapeutic index. Drugs with low therapeutic index have a narrow therapeutic window.
Drugs having 100% bioavailability
Drugs having 100% bioavailability include chlordiazepoxide, diazepam, lithium, metronidazole, phenobarbitol, salicylic acid, trimethoprin and valproic acid.
 howMed Know Yourself
howMed Know Yourself






I loved the article. ….