Electrophysiological Properties of heart
1. Automaticity
Automaticity is the property of the heart by which impulses are formed spontaneously. Impulses are formed by two main parts, i.e. SA node and AV node. SA node is mostly responsible, so called the pacemaker of heart.
2. Rhythmicity
Rhythmicity means that impulses are generated at regular intervals. The regular pattern in SA node is about 70/min, while that of AV node is 45/min. Purkinje fibers beat at rate of about 25/min. Any change in rhythmicity leads to cardiac arrhythmias.
3. Excitability
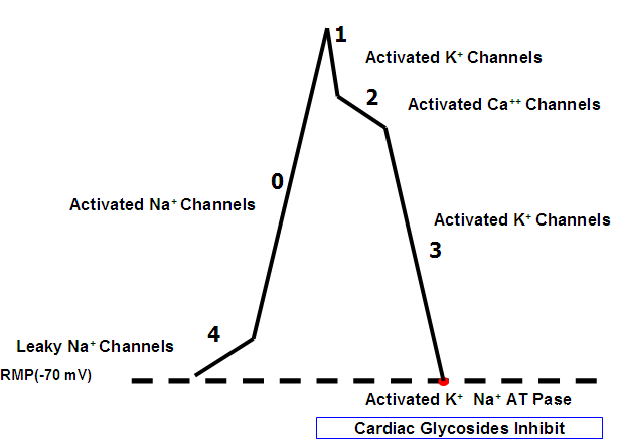
Excitability means the development of action potential in the heart. This is discussed in four phases:
Phase 0 Rapid influx of Na+ leads to depolarization. Normal resting potential is -70 mV. During phase 0 it rises to +30 mV.
Phase 1 Initial period of rapid re-polarization due to outflux of K+. Action potential changes from +30 to +10 mV.
Phase 2 The plateau phase. The delay in repolarization is due to the opening of voltage gated Ca++ channels. During this phase the action potential changes from +10 to -10 mV.
Ca++ channel blockers are used in the treatment of cardiac arrhythmias, which involve the activation of contractile machinery of heart due to the opening of Ca++ channels (SA and AV nodes are involved).
Phase 3 Phase of rapid repolarization. Rapid outflow of K+ occurs. Action potential changes from -10 to -70 mV.
After phase 3, full repolarization occurs. Na+ K+ ATPase is activated, which is responsible for bringing the ionic concentration back to normal (outflow of Na+ and inflow of K+).
Cardiac glycosides act by inhibiting the Na+ K+ ATPase pump.
Phase 4 No absolute inhibition of Na+ channels has occurs. Some inflow continues, once the potential reaches threshold, the cycle starts once again.
Most drugs act by blocking the various phases.
- Na+ channel blockers are used in cardiac arrhythmias.
- K+ channel blockers are used for increasing the excitability and refractory period
- Cardiac glycosides are used in cardiac failure to inhibit Na+ K+ ATPase.
4. Conductivity
Once action potential is generated, it is conducted to other parts of the heart. From SA node it travels to the atria, the AV node, the ventricles through the bundle of HIS (purkinje fibers). The conduction velocity is low in the atria (5 cm/sec) while it is very high in the ventricles (200 cm/sec).
5. Contractility
Contractility is the vigor of heart by which it pushes the blood into the systemic blood vessels. It is responsible for the development of cardiac output and maintenance of heart rate.
Compensatory Physiological Responses of Heart Muscle in CCF
When decrease in contractility occurs due to weakness of cardiac muscles or due to cardiac failure, the cardiac output decreases, as well as the heart rate.
1. Increased sympathetic activity.
To compensate this decrease, reflex mechanism of sympathetic activity occurs, by release of catecholamines. Increased sympathetic activity may cause sweating, palpitations, etc. Hypertrophy of heart may occur because of increased load.
2. Fluid retention and
3. Activation of renin-angiotensin system
Increased sympathetic activity also leads to increased fluid retention, and activation of rennin angiotensin system.
Note:
If the mechanisms listed above adequately restore cardiac output, then the heart failure is said to be compensated. If the adaptive mechanisms fail to maintain cardiac output, the heart failure is decompensated.
Drugs used in cardiac failure
1. Diuretics (alone or with K+ sparing diuretics)
i. Thiazides
Bendrofluazide, polythiazide etc
ii. Loop diuretic
Frusemide
2. ACE inhibitors
Captopril, enalapril etc
3. Angiotensin Receptor Blockers
Losartan, valsartan etc
4. Cardiotonic drugs
Cardiac glycosides
Bipyridine derivatives
Beta 1 selective agonists (Catecholamines)
Dobutamine, prenalterol
5. Vasodilators
Nitrates
6. Beta Blockers
Continue Reading
Digoxin and Digitoxin -Cardiac Glycosides
Bipyridine Derivatives -Milrinone and Inamrinone
 howMed Know Yourself
howMed Know Yourself





I am so glad as of getting this lecture note. if you are intersted please post such updated sciences regardig health by the above email adress. thanks!