• Diarrhea, derived from the Greek “to flow through,” is a common manifestation of gastrointestinal disease
• a consensus statement issued by the American Gastroenterological Association suggests that chronic diarrhea should be defined as a decrease in fecal consistency lasting for four or more weeks
• Based upon a commonly used definition (ie, the presence of excessive stool frequency) a reasonable approximation is that chronic diarrhea affects approximately 5 percent of the population
Causes of chronic diarrhea
1-OSMOTIC DIARRHEA
2-SECRETORY DIARRHEA
3-INFLAMMATORY DIARRHEA
4-MALABSORPTION SYNDROMES
5-MOTILITY DISORDERS
6-CHRONIC INFECTIONS
7-FACTITIOUS DIARRHOEA
OSMOTIC DIARRHEA
•CLUE-stool volume decreases with fasting,increased stool osmotic gap;
1-medicines-antacids,lactulose ,sorbitol
2-disaccrides deficiency –lactose intolerance
3-factitous diarrhea-magnessium
Secretory diarrhea
•CLUES-large volume>1l/d –little changewith fasting;normal osmotic gap
1-hormone mediated-VIPoma,carcinoid;zollinger ellison syndrom2-villous adenoma
2-Bile salt malabsorption(illeal resection,crohn,s colitis)
INFLAMMATORY CONDITIONS
•CLUES-fever,haematochezia,abdominal pain.
1-ulcerative colitis
2-crohn,s disease
3-microscopic colitis
4-malignancy
5-radiation enteritis
MALBSORPTION SYNDROMES
•CLUES-weight loss,abnormal laboratory values,fecal fat >10 gm/24 hr.
1-small bowel mucosal disorders;celiac sprue;tropical sprue;whipple disaes;crohn,s disease
2-lymphatic obstruction-lymphoma;carcinoid syndrome-pancreatic disorders-chronic panceartitis;pancreatic cancer.
3-bacterial overgrowth-motility disorders(diabetes mellitus),scleroderma
MOTILITY DISORDERS
•CLUES-systemic disorders or prior abdominal surgery
1-post surgical-post vagatomy
2-systemic disorders-scleroderma;diabetez mellitus
CHRONIC INFECTIONS
1-Prasites-Giardia lamblia,Entameba histolytica
2-AIDS-related
a-virus-cmv infection,HIV infection
b-Bacterial-Clostridium difficile ,mycobacterium avium complex
c-Protozoal-Microspirida,Cryptospiridium
HISTORY
•Characteristics of diarrhea-whether abrupt, gradual or congenital
•Pattern of diarrhea-continuous or intermittent
•Duration of symptoms,epidemiological factors like history of travel, exposure to potentially infected water or food, other family members being infected.
•Stool characteristics-watery,bloody or fatty.
•Abdominal pain.
•Weight loss.
•Aggravating and mitigating factors.
•Systemic diseases-diabetes mellitus,hyperthyroidism.acquaired immuno deficieny syndrome;collagen vascular disorders
EVALUATION
•A clear understanding of what led the patient to complain of diarrhea (eg, consistency or frequency of stools, the presence of urgency or fecal soiling) •Stool characteristics (eg, greasy stools that float and are malodorous may suggest fat malabsorption while the presence of visible blood may suggest inflammatory bowel disease)
•Duration of symptoms, nature of onset (sudden or gradual)
•Travel history
•Risk factors for HIV infection
•Weight loss
•Whether there is fecal incontinence (which may be confused with diarrhea) •Occurrence of diarrhea during fasting or at night (suggesting a secretory diarrhea)
•Family history of IBD
•The volume of the diarrhea (eg, voluminous watery diarrhea is more likely to be due to a disorder in the small bowel while small-volume frequent diarrhea is more likely to be due to disorders of the colon)
•The presence of systemic symptoms, which may indicate inflammatory bowel disease (such as fevers, joint pains, mouth ulcers, eye redness)
•All medications (including over-the-counter drugs and supplements)
•A relevant dietary (including possible use of sorbitol-containing products and use of alcohol)
•Association of symptoms with specific food ingestion (such as dairy products or potential food allergens)
•A sexual history (anal intercourse is a risk factor for infectious proctitis and promiscuous sexual activity is a risk factor associated with HIV infection
Physical examination
•findings suggestive of IBD (eg, mouth ulcers, a skin rash, episcleritis, an anal fissure or fistula, the presence of visible or occult blood on digital examination, abdominal masses or abdominal pain
• evidence of malabsorption (such as wasting, physical signs of anemia, scars indicating prior abdominal surgery)
• lymphadenopathy (possibly suggesting HIV infection),
•abnormal anal sphincter pressure or reflexes (possibly suggesting fecal incontinence)
•Palpation of the thyroid and examination for exopthalmus and lid retraction may provide support for a diagnosis of hyperthyroidism.
INVESTIGATIONS
•STOOL ANALYSIS;
A-24 hr stool collection for weight and quantitative fecal fat-stool weight greater than 300gm/24 hr cfm diarrhea;fecal fat >10 gm indicates malabsorption.
B-stool osmolality-stool osmolality less than serum implies that water or urine has been added to specimen;a stool ph less than 5.6 is consistent with carbohydrate malabsorption.
•C-stool laxative screen-in cases of laxative abuse stool mag,phosphate, and sulphate levels may be measured,phenolphthalein and bisacodyl are measured in stool water.
•D-Fecal leucocytes-implies inflammatory condition
•E-stool for ova and cysts-Giardia lamblia;E.histolytica,,cryptospiridium,cyclospora
BLOOD TESTS
- BLOOD CP
- LFT,S
- TSH
- ANEMIA-FOLATE AND B-12 ,IRON DEF
- HYPOALBUMINEMIA
- HYPONATREMIA AND NONIONIC GAP ACIDOSIS IN SECRETORY DIARRHEAS.
- •SEROLOGICAL TESTINGS FOR CELIAC SPRUE-IgG and IgA antigliadin Ab,sor tissue transglutaminase ab •Serum VIPLevels,calcitonin.gastrin
ENDOSCOPIC EXAM AND MUCOSAL BIOPSIES
•Sigmoidoscopy or cololscopy
•Upper GI endoscopy with small bowel biopsy e.g when malabsorption due to celiac disease or whipple disease;small intestinal aspirate in bacterial over growth
IMAGING STUDIES
•ABDOMINAL CT SCAN AND USG ABDOMEN IN CHRONIC PANCREATITIS •BARIUM RADIOGRAPHY IN CROHN,S DISEASE,SMALL BOWEL LYMPHOMA
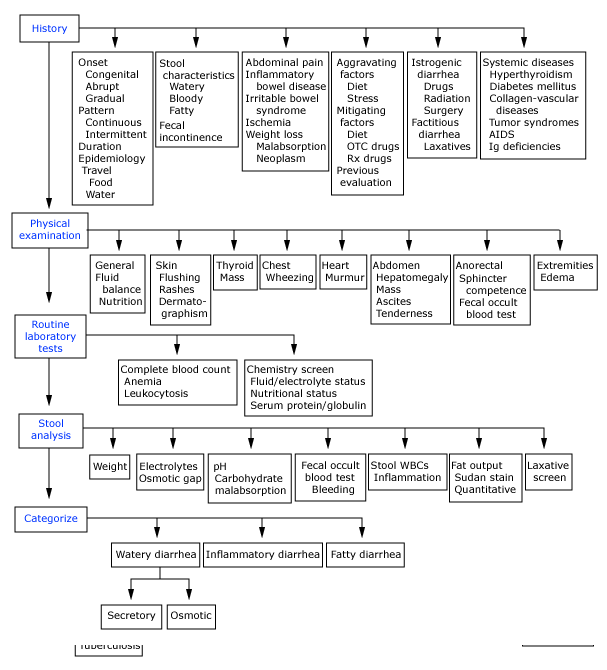
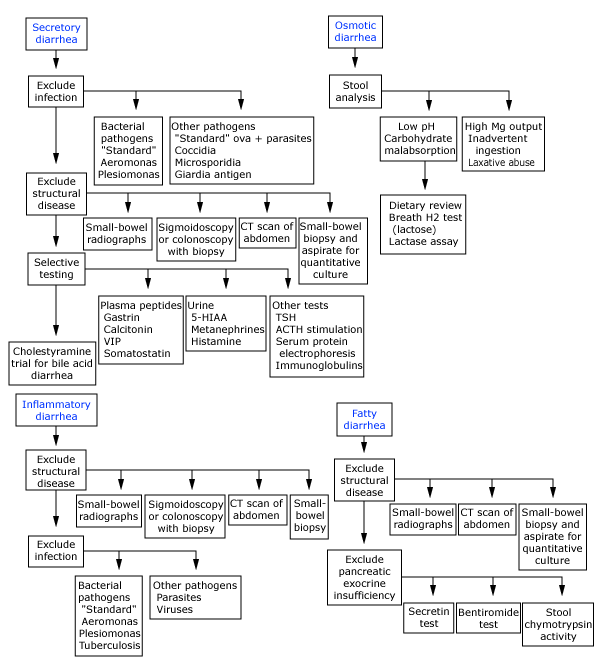
Diagnostic approach to chronic diarrhea
TREATMENT
•A number of antidiarrheals are available but they should be used in certain condtions only. Opiates are safe in chronic stable diarrhea.
•LOPERAMIDE
•DIPHENOXYLATE WITH ATROPINE
•CLONIDINE-SECRETORY DIARRHAES.
•OCTREOTIDE-NEUROENDOCRINE ASSOC
•CHOLESTYRAMINE-BILE SALT INDUCED DIARRHEA
Want a clearer concept, also see
Acute Diarrhoea
 howMed Know Yourself
howMed Know Yourself