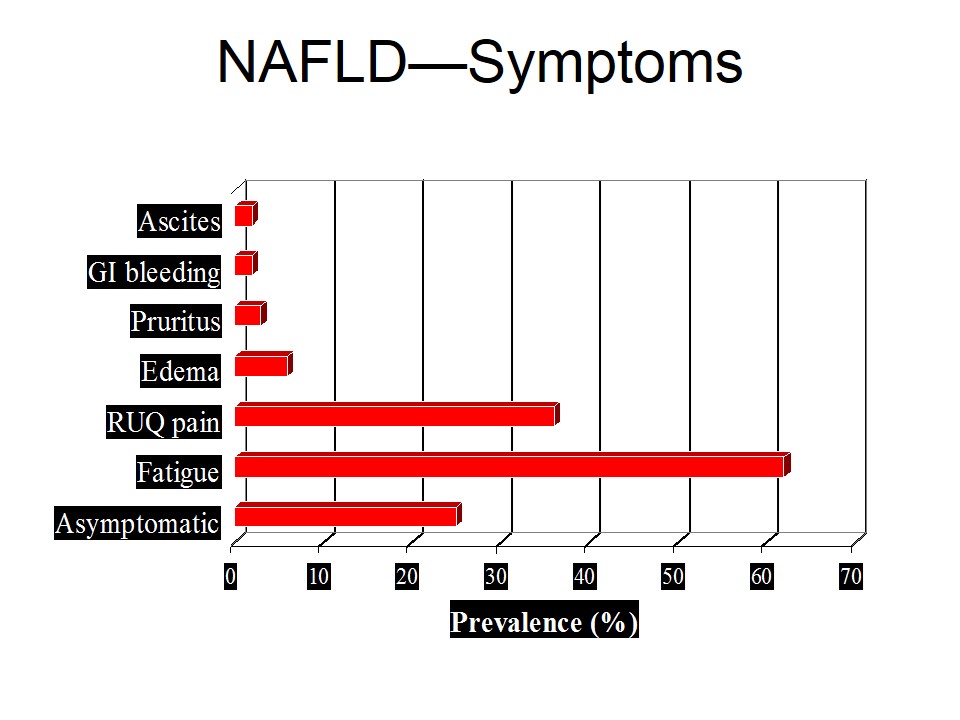
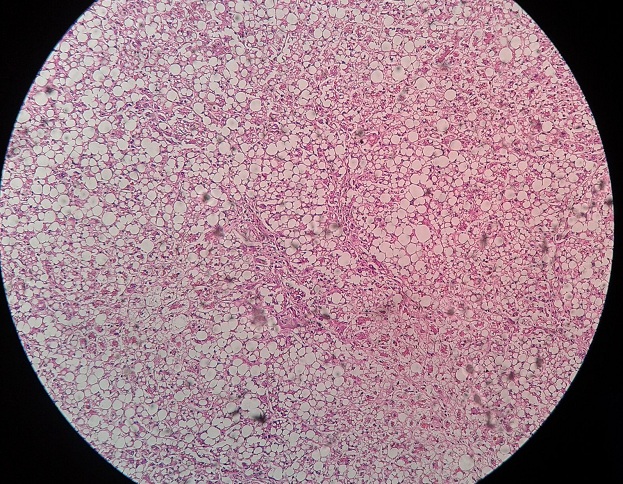
Fasting blood glucose level higher than 126 mg/dl or 7.0 mmol/l is labeled as hyperglycemia.
Fasting hyperglycaemia may occur in the following conditions:
1. Diabetes mellitus:
- Absence or insensitivity to insulin, leading to impaired glucose tolerance and hyperglycemia
2. Pancreatic disorders
a. Pancreatectomy :
- e.g.: trauma (road traffic accidents,penetrating abdominal injuries), Surgical removal of pancreas (for pancreatic tumor).
b. Haemochromatosis :
- Deposition of iron in islets cells within pancreas and destroying islet cells.
c. Chronic pancreatitis :
- Chronic inflammation of pancreas resulting in fibrosis & irreversible destruction of pancreatic parenchyma, e.g: Alcohol abuse, longstanding pancreatic duct obstruction.
d. Carcinoma of pancreas :
- Glucagonoma which is the tumour of Islet cells
3. Endocrine disorders
a. Cushing’s syndrome :
- Glucocorticoids will induce gluconeogenesis and inhibit glucose uptake by tissues causing hyperglycemia.
b. Acromegaly :
- Excessive secretion of Growth hormone causes increased gluconeogenesis
c. Thyrotoxicosis :
- Causes hyperglycemia by inducing glycogenolysis in liver,also increases the basal metabolic processes (activity/rates).
d. Phaeochromocytoma :
- Tumour of adrenal medulla causing hyperglycemia by secretion of catecholamines(epinephrine,norepinephrine),that cause gluconeogenesis.
4. Stress
Increased cortisol and adrenaline secretion leading to gluconeogenesis:
e.g:
- infections
- cerebrovascular accidents
- myocardial infarction (MI)
5. Iatrogenic
1. IV glucose infusions
2. Drugs
- Salicylates (analgesics)
- Oral contraceptives(steroid preparation)
- Steroids (used as antiallergic, anti inflammatory, replacement therapy for steroid deficiency)
-Thiazides (diuretics)
Note:
In MI stress, hyperglycaemia is fairly common. However, recent investigations indicate that many of these patients have diabetes mellitus (especially if the plasma glucose exceeds 10 mmol/L); thus, all stress hyperglycaemia patients should be investigated at a later date for possible diabetes mellitus.
 howMed Know Yourself
howMed Know Yourself