The thyroid gland produces hormones which regulate different processes and include:
- Tri-iodothyronine (T3) which is a follicular hormone and constitutes 7% of total
- Thyroxin (T4) which is also a follicular hormone constituting 93% of total
- Reverse T3, synthesized in the fetal thyroid and in peripheral tissues from T4. This is the biologically inactive form of thyroid hormones.
| Contents |
| Functions |
| Synthesis |
| Storage |
| Transport |
| Metabolism |
| Regulation |
Calcitonin is secreted from the parafollicular cells and is a Calcium lowering hormone. T4 is the major secretory product of the thyroid gland but T3 is biologically more active than T4.
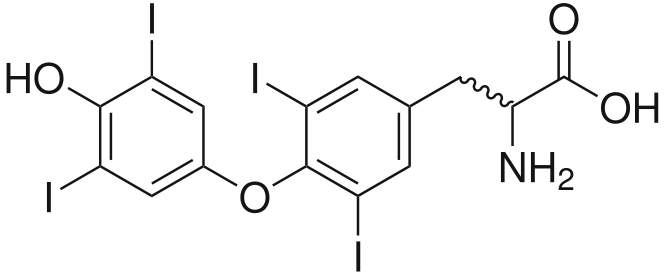
Structure of Thyroxine:
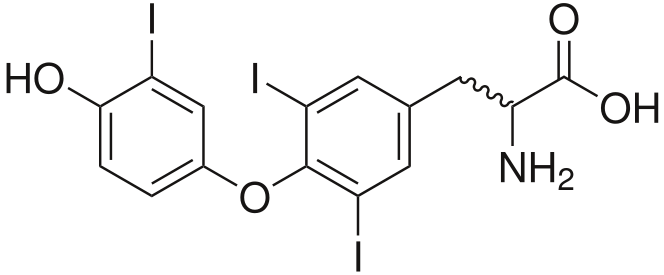
Structure of Tri-iodothyronine:
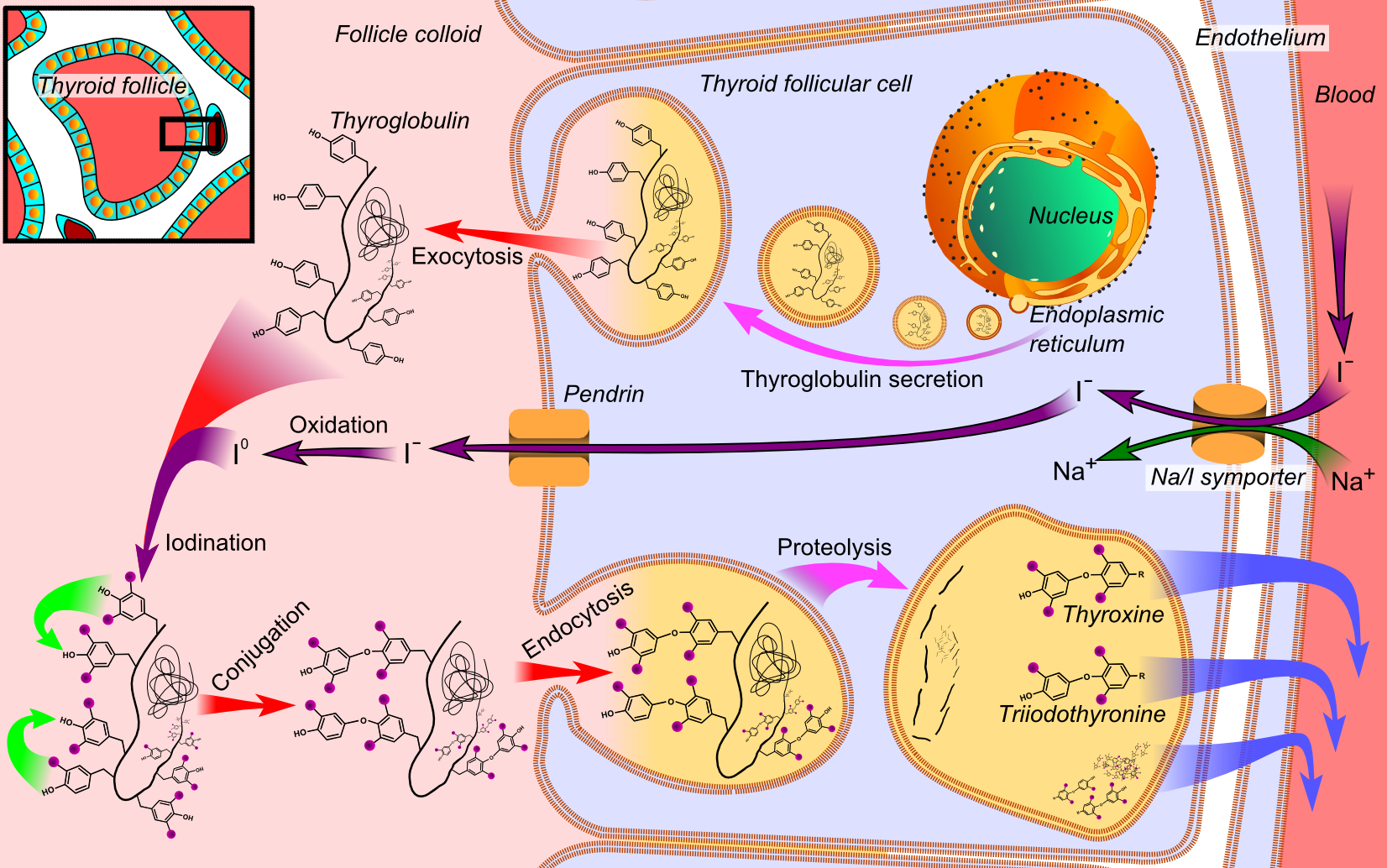
Synthesis:
Synthesis of thyroid hormones involve the following steps:
- Thyroglobulin synthesis
- Iodine uptake (Iodine trapping)
- Oxidation of iodide ions
- Iodination of tyrosine (organification)
- Coupling of MIT and DIT
- Release of thyroid hormone
Storage of Thyroid Hormones:
Each thyroglobulin molecule contains one to four T4 molecules. An average of one T3 molecule is present for 14 T4 molecules. The colloid of thyroid follicles have thyroid hormones sufficient for 2-3 month’s requirements.
Thyroid Hormones in Blood:
Approximately, 99.98% of T4 is bound to three serum proteins:
- Thyroid binding globulin~ 75%
- Thyroid binding prealbumin~ 15-20%
- Albumin~ 5-10%
Only about 0.02% of total T4 in the blood is unbound or free and only about 0.4% of total T3 in the blood is free.
Transport of Thyroid Hormones:
Total thyroid hormone is about 50-15 nmol/l out of which free thyroid hormone is only 40 pmol/l. 99% of the thyroid hormone is bound to the plasma proteins. Only 1% of thyroid hormones is in free form which is biologically active.
Metabolism of Thyroid Hormones:
T4 is converted by 5’deiodinase into:
- T3 which is the active form
- rT3 which is the inactive form
Inactivation takes place in the liver and the target tissues. Following steps are involved:
- Deiodination of MIT, DIT
- Deamination and Decarboxylation
- Conjugation to sulphates and glucuronic acid which is excreted in the urine.
The half life is approximately 6 days.
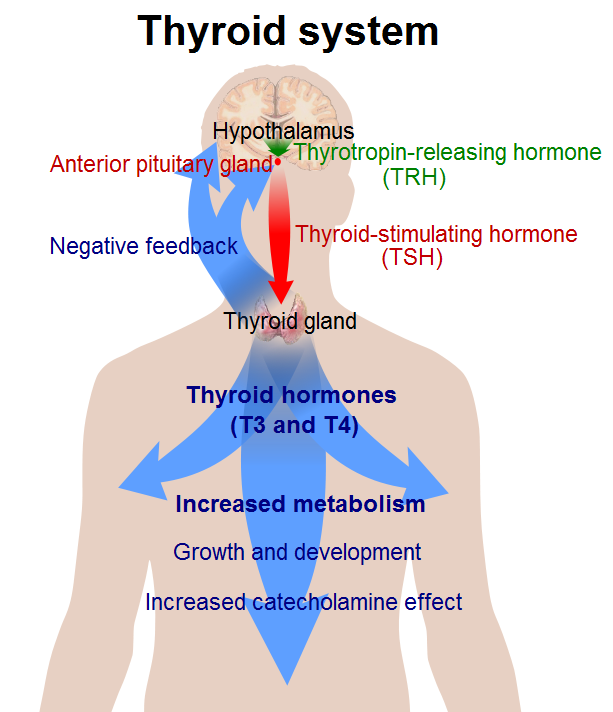
Regulation of Thyroid Hormone Synthesis:
The amount of thyroid hormone is precisely regulated. Stimulatory factors include:
- Thyroid stimulating hormone
- Thyroid stimulating immunoglobulin
- Increased thyroid binding globulin ( as in pregnancy)
Inhibitory factors include:
- Iodine deficiency
- Deiodinase deficiency
- Excessive iodine intake
- Perchlorate, thiocyanate (which inhibit the iodine pump)
- Polythiouracil (which inhibits the peroxidases)
- Decreased thyroid binding globulin (as occurs in liver diseases)
Exposure to cold causes increased TRH and TSH and increases BMR by 15 to 20%. Emotional reactions, too, cause increased TRH and TSH. Whereas excitement and anxiety causes a decrease in TRH and TSH.
Mechanism of Action:
Step 1: Conversion of T4 into T3 by 5’ Iodinase:
T4 is converted into its active form, which is T3 along with rT3. T3 is four times more active metabolically than T4.
Step 2: Entry of T3 into the nucleus of target cell to bind the nuclear receptor.
Step 3: The T3 receptor complex binds thyroid hormone regulatory element on the DNA to stimulate DNA transcription.
Step 4: Translation of newly transcribed mRNA into hundreds of new proteins.
Functions of Thyroid Hormones:
T4 has a long latent period and the peak action is observed 10-12 days after its injection into the body.
Its half life is 15 days and there is no action on BMR for 2 to 3 days. Some activity is observed for as long as 6 weeks to 2 months.
T3 acts rapidly after about 6-12 hours and the peak action is seen in 2-3 days.
The nature of induction of new proteins is specific to the target tissues. In most of the cases, Na+ K+ ATPase is induced which leads to an increased oxygen consumption while in myocardial cells, myosin, β adrenergic receptors and Ca++ ATPase are induced. In the liver and adipose cells, key metabolic enzymes are induced which alter the carbohydrate and protein metabolism.
In the target cells the T3 and T4 bind the intracellular receptors (T3 binds 90% and T4 binds 10%). The new proteins are synthesized which include:
- Na+ K+ ATPase
- Transport proteins
- Receptors
- Lysosomal proteins
- Proteolytic proteins
- Structural proteins
The thyroid hormones act on every organ system within the body. They act synergistically with growth hormone and somatomedins to:
- Promote bone formation
- Increase BMR, heat production and oxygen consumption
- Alter CVS, respiratory system to increase oxygen delivery to tissues.
The most important functions of thyroid hormones are:
- Calorigenesis and Increased BMR
- Growth and Development (Physical and Mental)
- Activation of specific body mechanisms (including metabolism)
Calorigenesis and Increased BMR
Muscles are affected the most by the thyroid hormones. (There is non calorigenic effect on the brain, anterior pituitary, lymph nodes and spleen). About 40% of the total heat produced in the tissues is by thyroid hormones. They increase the number and size of the mitochondria as well as their activity and lead to an increased ATP formation.
They cause uncoupling of oxidative phosphorylation and increase the BMR by 60-100% normal. An increased activity of Na+ K+ ATPase is observed in most of the cells.
Effect on Bones and Muscles:
TH is critical for normal development of the skeletal system as well as the musculature. In growing children, it enhances the growth while in hypothyroid children, growth retardation, rapid maturation of bones and stunted growth is observed.
Effect on Brain:
Thyroid hormones promote growth and development during fetal life and a few years of the postnatal life. TH is essential for the normal brain development and regulates the synaptogenesis, neuronal integration, myelination and cell migration. Decreased T4 in fetus of after birth causes cretinism, which results in retarded growth and maturation of the brain. These children remain mentally deficient throughout life.
Permissive Actions:
TH increases sensitivity of target tissues to catecholamines, thereby elevating lipolysis, glycogenolysis and gluconeogenesis.
Metabolic Functions:
All metabolic functions are due to an overall increase in the cellular metabolic enzymes.
Effect on Carbohydrates:
- Increase absorption of glucose in small intestine
- Increase uptake of glucose by cells
- Increase glycolysis
- Increase glycogenolysis
- Increase gluconeogenesis
Hyperglycemia and insulin secretion leads to thyroid diabetes.
Effect on Fats:
All aspects of fat metabolism are enhanced. Increased lipolysis leads to an increase in free fatty acids in the plasma and decreased fat stores in the body.Triacylglycerols are broken into glycerol and free fatty acids. Free fatty acids undergo beta oxidation in the liver and lead to decreased cholesterol in the plasma.
Effect on Proteins:
Thyroid hormones have an anabolic effect in low doses while in high doses, they have a catabolic effect.
Effect on Minerals:
Thyroid hormones cause osteoporosis and decalcification in large doses.
Effect on Vitamins:
Increased thyroid hormones cause an increased requirement of vitamins, as these are part of the enzymes and co-enzymes.
Systemic Actions:
Body Weight:
Excess T4 leads to a decrease in body weight. A decrease leads to opposite results.
Central Nervous System:
Excess thyroid hormones cause rapid cerebration, nervousness, anxiety, extreme worry, psychoneurotic tendency and paranoia.
Sleep:
Thyroid hormones cause increased feeling of tiredness but difficulty to sleep, due to the fact that they cause increased excitability of synapses (as occurs in hyperthyroidism).
Muscles:
Thyroid hormones cause fine tremors at the rate of 10-15 times per second. This is because of increased activity of neuronal synapses in motor neurons of spinal cord.
Respiratory System:
Thyroid hormones cause an increase in rate and depth of breathing due to and increase in BMR. They also cause increased utilization of oxygen and more formation of carbon dioxide.
Cardiovascular System:
Thyroid hormones cause an increase in cardiac output (approximately 60% above normal). They cause an increase in the blood flow to the tissues, organs and the skin (to loose greater heat of metabolism). An increase in heart rate and contractility is observed due to the direct effect of cardiac output as well as the up regulation of beta adrenergic receptors. Excessive T4 may cause protein catabolism of myocardium and cardiac decompensation, leading to death. The mean arterial pressure remains normal although an increase in systolic blood pressure is observed along with decrease in diastolic blood pressure. The pulse pressure rises.
GIT:
Thyroid hormones cause an increase in motility and secretions leading to diarrhea. An increased appetite and food intake is observed. In hypothyroidism, constipation is usually seen.
Endocrine Glands:
An increase in secretions of most endocrine glands is caused by thyroid hormones e.g. Insulin, parathyroid hormone, adrenocorticotrophic hormone, glucocorticoids.
 howMed Know Yourself
howMed Know Yourself