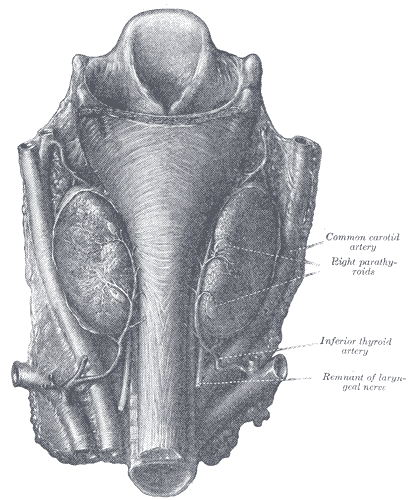
Four parathyroid glands are normally present, two embedded in the superior pole of the thyroid and two in the inferior poles. These are richly vascularized and size is about 3x6x2 mm.
| Contents |
| Action |
| Mechanism |
| Regulation |
| PTHrP |
The parathyroid glands contain two types of cells:
1. Chief Cells:
Chief cells synthesize and secrete the parathytroid hormone.
2. Oxyphil Cells:
Oxyphil cells are less abundant and larger in size. Their function is unknown.
The parathyroid hormone is a linear polypeptide with a molecular weight of about 9500, containing 84 amino acid residues. It is synthesized as preproparathyroid hormone, conataining 115 amino acid residues, It is then converted into proparathyroid hormone containing 90 amino acid residues, and finally into the parathyroid hormone.
The parathyroid hormone also exists in the storage vesicles, which serve as several hour supply of the hormone. The normal plasma level of intact parathyroid hormone is 10-55 pg/mL. Its half life is approximately 10 minutes. It is secreted as a polypeptide rapidly cleaved by the Kupffer cells, located in the liver, into fragments. These fragments are then cleared by the kidneys.
Actions:
- The parathyroid hormone acts directly on bones to increase bone resorption and mobilize Ca++.
- It increases the reabsorption of Ca++ in the distal tubules.
- It increases the formation of 1,25-dihydroxycholecalciferol, and this increases Ca++ absorption from the intestines.
- It stimulates both the osteoblasts and the osteoclasts.
- It increases phosphate excretion in the urine and thereby depresses plasma phosphate levels.
- It also has phosphaturic action by the decrease in reabsorption of phosphate in the proximal tubules.
Mechanism of Action:
There are three different types of parathyroid hormone receptors:
1. hPT/PTHrP receptor:
Receptor binds both the parathormone and the parathyroid hormone related protein(PTHrP).
2. hPTH2-R:
Second receptor which does not bind PTHrP and is found in the brain, placenta and pancreas.
3. CPTH:
Third receptor which reacts with the carboxyl terminal rather than the amino terminal of PTH.
The first two receptors are coupled to excitatory G protein, and via this heterotrimeric G protein they activate the adenylyl cyclase, increasing intracellular cAMP.
The hPTH/PTHrP receptor also activates phospholipase C, increasing intracellular Ca++ and activating protein kinase C.
Regulation of Secretion:
The circulating ionized calcium provides a negative feedback. There is simple inverse linear relationship between plasma Ca++ and plasma PTH. The activation of cell membrane Ca++ receptor also inhibits PTH secretion.
1,25-dihydroxychoelcalciferol acts directly on the parathyroid glands to decrease preproPTH mRNA. Increased plasma phosphate stimulates PTH secretion. Magnesium is required to maintain normal parathyroid secretory responses.
Parathormone and Kidneys:
Parathyroid hormone induces phosphaturia, decreased calcium excretion and formation of 1,25 dihydroxycholecalciferol.
Parathyroid Hormone Related Protein (PTHrP)
PTHrP is another protein with PTH activity. It is produced by many different tissues in the body and consists of 140 amino acid residues. It is encoded by a gene on human chromosome 11. PTHrP and PTH have marked homology at their amino terminal ends. Both of them bind to hPTH/PTHrP receptor but their physiological effects are very different. PTHrP has marked effect on the growth and development of cartilage.
 howMed Know Yourself
howMed Know Yourself