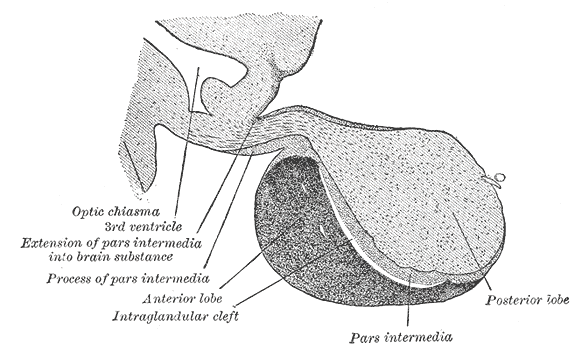
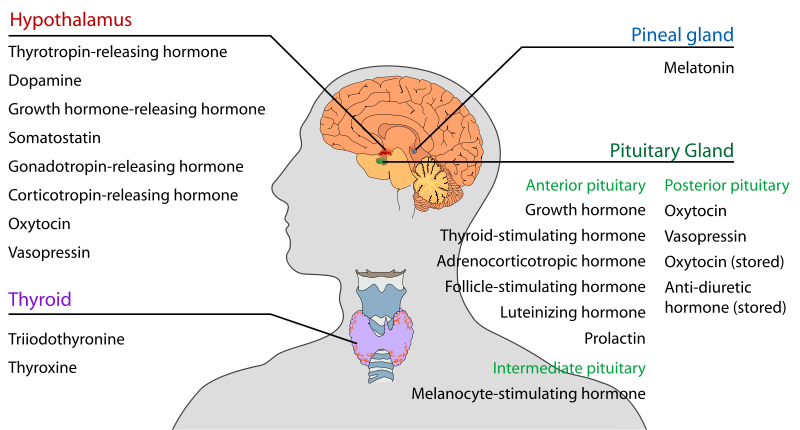
Pituitary is and endocrine gland located within the sella turcica, residing inside the skull. It is about one cm in diameter and weighs about 0.5 -1 gm. It is connected through the pituitary stalk with the hypothalamus.
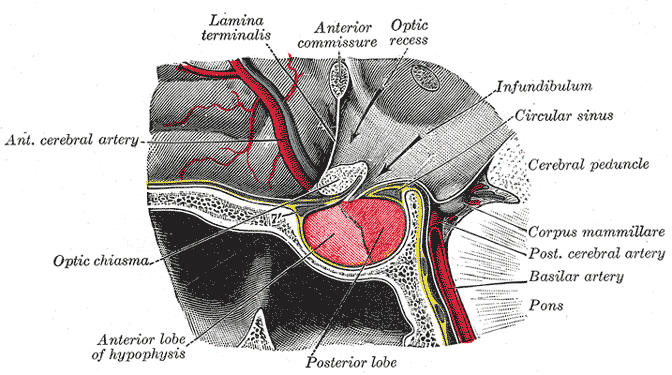
Grey’s Anatomy 20th edition
Portions:
Pituitary gland is divided into three portions:
a. Adenohypophysis or anterior pituitary (develops from Rathke’s pouch)
b. Neurohypophysis or posterior pituitary (neural tissue outgrowth from hypothalamus)
c. Pars intermedia
Grey’s Anatomy 20th edition
Anterior Pituitary gland
Cell Types and Hormones:
Anterior pituitary consists of five different cell types producing six hormones. These include:
1. Somatotropes producing the human growth hormone (hGH).
2. Corticotropes producing adrenocorticotropic hormone (ACTH)
3. Thyrotropes producing thyroid stimulating hormone (TSH)
4. Gonadotropes producing luteinizing hormone (LH) amd follicle stimulating hormone (FSH).
5. Lactotropes producing prolactin (PRL)
Control of Anterior Pituitary Secretions
Anterior pituitary secretions are regulated by the hormones from hypothalamus, acting through the hypothalamic-hypophysial portal system. These include:
a.Thyrotropin releasing hormone (TRH), stimulating the production of thyroid stimulating hormone.
b. Corticotropin releasing hormone (CRH), stimulating the production of adrenocorticotropic hormone.
c. Growth hormone releasing hormone (GHRH), stimulating the production of growth hormone.
d. Growth hormone inhibitory hormone (GHIH), inhibiting the production of growth hormone.
e. Gonadotropin releasing hormone (GnRH), stimulating the production of FSH and LH.
f. Prolactin inhibitory hormone (PIF), inhibiting the release of prolactin.
Growth hormone
Growth hormone, also known as the somatotropic hormone or somatotropin, is produced by the somatotrophs. It is an important hormone for growth and development.
Functions of Growth Hormone
Effects on Growth:
Growth hormone effects growth by:
a. Increasing the number of cells.
b. Increasing the size of the cells.
c. Increasing the differentiation of cells
Metabolic Effects
Growth hormone has metabolic effects on
a. Proteins
Growth hormone decreases the utilization of proteins in the body by:
1. Increase in protein deposition in the cells
2. Increase in DNA transcription
3. Increase in RNA translation
4. Increase in amino acid transport
5. Decrease in protein catabolism
b. Carbohydrates
A decrease carbohydrate utilization is observed along with a decrease in glucose uptake by the tissues, accompanied by increased glucose production by the liver. An increase in insulin production is also observed, but it is unable to mediate its effects of decreasing glucose levels in blood (this is attributed to the increased levels of free fatty acids, which hinder the effects of insulin). Thus growth hormone is a diabetogenic hormone producing pituitary diabetes (due to overproduction of glucose and decreased utilization).
c. Fats
Growth hormone increases the utilization of fats and increases fat mobilization. It causes an increase in the levels of free fatty acids in the plasma. The levels of acetyl Co-A (produced from the free fatty acids) also rise in the body, thus fats are used for providing energy to a greater extent, while carbohydrates are spared. Thus, under the influence of growth hormone, an increase in lean body mass is observed. Increased production of acetyl Co-A also lead to increased formation of ketone bodies, thus causing ketosis.
Effects on bones
Growth hormone causes:
a. increased deposition of proteins by chondrocytes and osteoblasts
b. increased reproduction of chondrocytes and osteoblasts
c. conversion of chondrocytes into osteocytes
Mechanisms of bone growth
There are two ways in which bones grow:
a. Longitudinal growth
Longitudinal growth involves the increase in bone length which occurs at the epiphyseal plates. The chondrocytes undergo mitosis and there is deposition of new cartilage. Ossification of new cartilage results in the formation of new bone. There is, thus, elongation of shaft in longitudinal growth.
b. Horizontal growth
The horizontal growth involves the increase in bone thickness. The osteoblasts deposit new bone while the osteoclasts remove the old bone. The rate of deposition of bone is greater than the rate of resorption. There is ,thus, increase in thickness of the shaft.
Somatomedins:
Somatomedins are small proteins synthesized in liver under the influence of growth hormone. These are also known as Insulin-like growth factor (IGF). They increase all aspects of bone growth. Somatomedins have longer half life than growth hormone. There are four major somatomedins, but the most important is the somatomedin C (IGF-I).
African pygmies have a congenital inability to synthesize somatomedin C. Their plasma growth hormone levels are normal or high, but they remain small statured. The Levi-Lorain dwarves have the same problems.
Regulation of GH
Hypothalamus releases growth hormone releasing hormone (GHRH) which increases the production of growth hormone. It also releases growth hormone inhibitory hormone (GHIH), which inhibits the production of growth hormone.
The GHRH acts through the cAMP dependent 2nd messenger system.Short term influences are mediated through the calcium influx while the long term effects through the transcription and new hormone synthesis.
Growth Hormone and Aging
Growth hormone is also known as anti-aging hormone as is evident from the growth hormone levels during different periods of life:
a. 5-20 yrs —- 6 ng/ml
b. 20-40 yrs — 3 ng/ml
c. 40-60 yrs — 1.6 ng/ml
Anti aging actions of GH
Growth horomone has anti aging actions due to the fact that it increases the deposition of proteins, at the same time decreasing the deposition of fats. Person has a feeling of increased energy.
Panhypopituitarism
Panhypopituitarism can occur in children as well in adults. In children it may be congenital or due to tumors, while in adults it is due to tumors or thrombosis of pituitary vessels (Shehaan’s syndrome).
Effects
Panhypopituitarism causes:
b. Decreased glucocorticoids
c. Decreased gonadotropins
Dwarfism
Dwarfism is due to:
a.Panhypopituitarism
b. Lack of GH
c. Lack of somatomedins
Features
Features include stunted growth but it is proportionate (unlike cretinism). Person is mentally normal.
Treatment
Treatment involves growth hormone injections
Gigantism
Increase GH before adolescence results in gigantism.
Features
Features involve increased growth of body tissues, increased height accompanied by hyperglycemia/ diabetes.
Acromegaly
Increase GH after adolescence results in acromegaly. The person can not grow taller but soft tissues continue to grow and bones grow in thickness.
Features:
Features include:
a. Enlarged hands and feet
b. Slanting forehead
c. Protruded lower jaw
d. Kyphosis
e. Enlarged nose, tongue, kidney and liver.
Posterior Pituitary Gland
Posterior pituitary gland is also known as neurohypophysis because it is the neural tissue outgrowth from hypothalamus. Pituicytes (glial like supporting cells) and nerve fibers from supraoptic and paraventricular nucleus of hypothalamus are present within it.
Hormones
Posterior pituitary glands releases two hormones:
a. Antidiuretic hormone (ADH) or Vasopressin (5/6 comes from supraoptic nucleus of hypothalamus, 1/6 from paraventricular nucleus)
b. Oxytocin (5/6 from paraventricular nucleus, 1/6 from supraoptic nucleus)
Carrier proteins are the neurophysins, which carry the hormones from hypothalamus to posterior pituitary. Hypothalamus controls the release of hormones from the posterior pituitary gland.
Antidiuretic hormone (ADH) or Vasopressin
Antidiuretic hormone or vasopressin is secreted from the hypothalamus. 5/6 is produced in the supraoptic nucleus and 1/6 in paraventricular nucleus.
Actions
a. Osmotic regulation:
ADH regulates osmolarity within the body.
b. Vasoconstriction
ADH plays a role in maintainence of blood pressure by vasoconstriction.
Regulation of ADH secretion
Osmotic regulation
Osmoreceptors are present within hypothalamus or around it. Hyperosmolar extracellular fluid pulls out fluid from the osmoreceptos, which results in shrinkage of osmoreceptors. The shrinkage of osmoreceptors signals ADH secretion from the hypothalamus, which restores the normal osmolarity.
Stretch receptors are present within the right atria. They are excited by overfilling. Their excitation inhibits ADH secretion (volume reflex) which decreases blood pressure. Decreased stretch of baroreceptors results in an increased ADH secretion.
Mechanism of Action of ADH:
On Renal Tubules
ADH acts on collecting tubules and collecting ducts. It binds to its receptors (V2), which results in activation of adenylyl cyclase. Activated adenylyl cyclase results in the formation of cAMP, which causes activation of cAMP dependent protein kinases. Activated protein kinases cause phosphorylation of aquaporins, which results in insertion of aquaporins into cell membrane. This increases permeability for water.
On Vascular Smooth Muscles
ADH binds to its receptors (V1) resulting in activation of Phospholipase C. It causes formation of IP3 & DAG which releases Ca++ from intracellular stores. This causes activation of Protein kinase C which results in phosphorylation of cell proteins producing cell response.
Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH)
In this syndrome there is excessive secretion of ADH.
Cause:
Cause might be:
a. Small cell carcinoma of lung
b. Brain tumors
c. Head trauma
Pathophysiology
Increased ADH causes increased reabsorption of water resulting in hyponatremia and overhydration. This increases ICF volume and decreases ICF osmolarity.
Diabetes Insipidus
Excessive secretion of urine due to either decreased production of ADH or lack of response to it is known as diabetes insipidus. There are two types of diabetes insipidus:
a. Cranial- due to less secretion of ADH
b. Nephrogenic- due to diminished response to ADH
Pathophysiology:
There is inability to secrete ADH or respond to it, as a result of which large amount of dilute urine is excreted, resulting in dehydration and increased ECF osmolarity.
Oxytocin
Oxytocin causes uterine contractions and milk letdown phenomenon.
Uterine Contractions:
As a result of stretching of cervix, signals are sent to the hypothalamus, which causes the release of oxytocin from posterior pituitary gland. The oxytocin released causes contraction of uterine muscles.
Milk ejection/milk let down
The stimulus is suckling by the baby which sends sensory signals to hypothalamus resulting in release of oxytocin from posterior pituitary gland. Oxytocin contracts myoepithelial cells, causing milk ejection.
 howMed Know Yourself
howMed Know Yourself