Shigella is a genus of gram negative rods, which are non-spore forming, non-encapsulated and non-motile bacteria, responsible for causing enterocolitis and dysentery.
Pathogenesis
Route of Entry
Route of entry is mainly by feco-oral route. Primary factors for transmission are the 4 F’s:
1. Fingers
2. Flies
3. Food
4. Feces
Only a small dose of bacteria is required (around 100 organisms) because they are resistant to hydrochloric acid present in stomach. Shigella causes disease exclusively in GIT. It produces dysentery by invading the cells of the mucosa of the distal ileum and colon. It is responsible for causing ulceration with local inflammation. It rarely penetrates through cell wall or enter blood stream.
Only ‘O’ antigen is present.
Virulence Factors
• Endotoxin – lipopolysaccharide
• Shiga-like Toxin (SLT), which is an enterotoxin
• Enterotoxins
Enterotoxins inhibit host cell protein synthesis.
Predisposing factors
- Improper sewage disposal
- Poor hygiene
Diseases are more common among children and elderly. Also in mental hospitals.
Lab Diagnosis
Specimen
• Fresh fecal specimen
• If a delay is anticipated then suitable transport medium should be used.
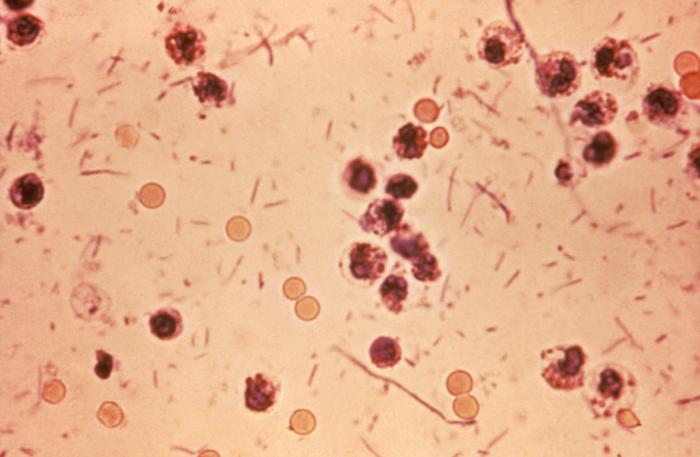
Microscopy
Following features are seen on microscopy:
• Gram negative rods
• Non-spore forming
• Non-encapsulated
• Non- motile
• Facultative
Culture
Incubation period is 1-4 days.
1. XLD agar, red -pink colonies are formed, without black centers
2. MacConkey’s agar, colorless colonies are formed
3. Methylene blue stain when applied on fecal sample, stains shigella, salmonella or campylobacter
Biochemical Tests
Triple sugar iron (TSI) agar
On triple sugar iron, alkaline slant and acidic butt is produced. No gas or H2S is produced.
- Lactase Negative
- H2S Negative
- Urease Negative
- Oxidase Negative
- Citrate Negative
- Lysine Decarboxylose
Serological Tests
• Slide agglutination test
• PCR
Diseases
1. Enterocolitis
2. Dysentery
Clinical symptoms
• Fever
• Abdominal cramps
• Diarrhea, which is watery at first, followed by stools with blood, mucus and pus cells
Treatment
- Fluid and electrolyte replacement
- In mild cases no antibiotics are required
- In severe cases Ciprofloxacin is used
- Antiperistaltic drugs are contraindicated
 howMed Know Yourself
howMed Know Yourself